Rapid Retrieval of Live, Infectious Pathogens from Clinical Samples

Complete the form below to unlock access to ALL audio articles.
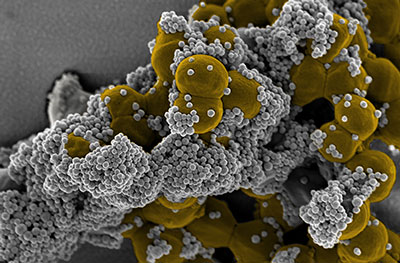
Pinpointing the type of bacteria that are at the root of an infection in clinical samples removed from living tissues, such as blood, urine or joint fluids, to quickly identify the best anti-microbial therapy still poses a formidable challenge. The standard method of culturing can take days to reveal pathogens, and they often fail to bring them to light altogether.
A team lead by Donald Ingber, M.D., Ph.D., at the Wyss Institute for Biologically Inspired Engineering at Harvard University now reports a method in PLoS, which enables the rapid isolation and concentration of infectious bacteria from complex clinical samples to help speed up bacterial identification, and it should be able to accelerate the determination of antibiotic susceptibilities as well.
"We leveraged FcMBL — the genetically engineered pathogen-binding protein we developed for our sepsis therapeutic device program — to develop a fast and simple technology to help overcome this diagnostic roadblock,” said Ingber, who is the Wyss Institute’s Founding Director, the Judah Folkman Professor of Vascular Biology at Harvard Medical School and the Vascular Biology Program at Boston Children’s Hospital, and Professor of Bioengineering at the Harvard John A. Paulson School of Engineering and Applied Sciences. “Using clinical samples of joint fluids, we were able to show that this method can be used to quickly and efficiently isolate bacterial pathogens for various kinds of subsequent analysis, including PCR, which is commonly used for molecular diagnostics in clinical laboratories.”
FcMBL is a recombinant form of the human blood protein, Mannose Binding Lectin (MBL), fused to a portion of the antibody Fc domain. The engineered protein can bind to more than 90 different microbial pathogens and toxins, ranging from fungi to bacteria, viruses and parasites and it even binds antibiotic-resistant organisms.
Earlier studies by Ingber’s team have used FcMBL as the key component of a dialysis-like blood cleansing device for sepsis therapy. The Wyss Institute’s efforts focusing on pathogen capture in different applications are funded by the Defense Advanced Research Project Agency (DARPA).
"Given our exciting results pulling pathogens out of flowing blood using FcMBL, we asked whether we could also capture live bacteria from clinical samples for detailed molecular analysis," said Michael Super, Ph.D., a Wyss Senior Staff Scientist who helped lead this research effort.
As a starting point, the team investigated samples obtained from patients with infections of joints or joint replacements, where the pathogen Staphylococcus aureus can lead to painful inflammation or form bacterial biofilms that often render artificial surfaces into health hazards, leading to joint failure or sepsis.
"We showed that FcMBL-coated magnetic beads bound to 12 clinical S. aureus isolates after these were cultured from infected joint fluids and that we could isolate them using magnets; however, in our initial studies, the FcMBL-beads did not bind S. aureus directly in infected joint fluids. We then realized that immune cells and factors in patient samples mask the sugar molecules on bacteria that FcMBL usually binds to. This, together with the viscous nature of the complex clinical samples impeded the efficacy of the fusion protein," said Super.
The team remedied both problems with a cocktail of enzymes. When joint samples are pre-treated with this cocktail, protease enzymes eliminated the interfering immune factors to expose bacterial surface sugars for FcMBL binding, while another enzyme in the mix, hyaluronidase, breaks down a class of large polymers that are responsible for the high viscosity of joint fluids.
"Using this approach, we were able to isolate and concentrate pathogenic S. aureus cells in only 2 hours, which could make a tremendous difference in clinical settings, especially in cases where pathogens can not be cultured straight out of the sample. This could let us fast-track the best antimicrobial treatment option in often critical situations," said Alain Bicart-See, M.D. the study’s first author who as a Wyss Institute Visiting Scholar collected the samples at Hospital Joseph-Ducuing in Toulouse, France where he specializes in infectious diseases.
After their isolation, pathogenic bacteria can be molecularly identified with methods that either look for the presence of DNA snippets specific for candidate pathogens or identified by mass spectrometry, a technique that can survey all pathogenic proteins present in a sample. The Wyss researchers also think that the method will facilitate antibiotic susceptibility testing since bacteria retrieved with the method are alive.
"This isolation technique should be able to be used to rapidly identify pathogens in other clinical samples including blood, urine, sputum, and cerebral spinal fluid, and thus, it will hopefully shorten the time required for physicians to select the optimal therapy. In addition to saving more lives, this new method also should reduce the use of broad-spectrum antibiotic therapies, or suboptimal regimens, and thereby, decrease development of antibiotic-resistant organisms that become a more general threat in the long run," said Ingber.

