Nitrosamine Impurities in Medicines

Complete the form below to unlock access to ALL audio articles.
In 2018, a nitrosamine impurity (N-nitrosodimethylamine or “NDMA”) was detected in several pharmaceutical drugs containing the active ingredient valsartan, which resulted in a voluntary product recall. The unexpected discovery of these impurities has subsequently fueled the development of new manufacturing requirements for these medications, and pharmaceutical companies have had to take precautionary measures to mitigate the risk of producing nitrosamines during drug synthesis.
Here, we take a closer look at nitrosamines, how they are created, the related health concerns and examples of nitrosamine impurities that have been detected.
What are nitrosamines?
Nitrosamines, also referred to as N-nitrosamines, possess a nitroso (–NO) group attached to nitrogen, and are formed when nitrates or nitrites react with secondary or tertiary amines.
Although nitrosamines are present in some foods (e.g. meat, dairy products and vegetables) and drinking water supplies at low levels, their presence in pharmaceutical products is considered, by the regulatory agencies, to be unacceptable.
What are the health concerns?
Nitrosamine impurities have been shown to be probable human carcinogens, based on animal studies, and are therefore deemed to be a health concern.
Dimethylnitrosamine (DMN), now more commonly known as NDMA, was first reported to be carcinogenic in rats, in a study by Magee and Barnes in 1956. DMN was added to the diet of male and female albino rats. In the rats given DMN, the authors reported that “a very high incidence of hepatic tumors occurred, many with metastatic spread”.
Subsequent work by Magee and Barnes in 1967, identified several additional nitroso compounds as being carcinogenic, including N-nitrosodiethylamine (NDEA). NDEA and NDMA have both been shown to cause tumors in several species of animal, at various tissue sites, via several different routes of exposure.
 Figure 1: Structure of NDEA and NDMA compounds.
Figure 1: Structure of NDEA and NDMA compounds.
Since NDEA and NDMA (Figure 1) were listed in the Second Annual Report on Carcinogens in 1981, additional studies performed using various preclinical models have further demonstrated their carcinogenic properties.
More information on the carcinogenic effects of NDEA, NDMA and other nitrosamines can be found here.
Nitrosamines are considered “known mutagenic carcinogens” (Class 1 impurities) by the ICH M7(R1) Guideline.
Potential causes of nitrosamine formation
The European Medicine Agency (EMA) lists several potential causes for the presence of nitrosamines in pharmaceutical drugs:
- Use of sodium nitrite* in the presence of secondary or tertiary amines or quaternary ammonium salts within the same or different process steps (if carryover can occur).
- Use of sodium nitrite* in combination with reagents, solvents, and catalysts, which are susceptible to degradation to secondary or tertiary amines, within the same or different process steps (if carryover can occur).
- Use of contaminated raw materials in the active pharmaceutical ingredient (API) manufacturing process.
- Use of recovered materials (e.g. solvents) including recovery outsourced to third parties who are not aware of the content of the materials they are processing, and routine recovery processes carried out in non-dedicated equipment.
- Use of contaminated starting materials and intermediates supplied by vendors that use processes or raw materials that could allow for the formation of nitrosamines.
- Cross-contamination events due to different processes run on the same manufacturing line and due to operator-related errors.
- Degradation processes of starting materials, intermediates and drug substances, including those induced by inherent reactivity in combination with carry-over of sodium nitrite*(can occur during finished product formulation or storage).
- Use of certain packaging materials.
*or other nitrosating agents
Daily intake limits for nitrosamines
Numerous regulatory authorities, including the US Food and Drug administration (FDA) have set internationally recognized daily intake limits for nitrosamines (Table 1). If an approved drug is shown to contain levels of nitrosamines above the allowable daily intake limits, the FDA recommends that the drug be recalled. The FDA also advises that “nitrosamine impurities may increase the risk of cancer if people are exposed to them above acceptable levels and over long periods of time.”
Table 1: Interim allowable daily intake limits for nitrosamine impurities.
| Chemical Name | Abbreviation | Allowable Daily Intake (AI) |
| N-nitrosodimethylamine | NMDA | 96.0 ng/day |
| N-nitrosodiethylamine | NDEA | 26.5 ng/day |
| N-nitroso-N-methyl-4-aminobutyric acid | NMBA | 96.0 ng/day |
| N-nitrosodiisopropylamine | DIPNA | 26.5 ng/day |
| N-nitrosoethylisopropylamine | EIPNA | 26.5 ng/day |
According to the World Health Organization (WHO), in instances where nitrosamines have been positively identified in pharmaceutical products, regulatory agencies should take the following steps:
- Confirm the levels of nitrosamine in the identified product, using either national testing laboratories or self-declarations from the suppliers themselves. Appropriate test methods should be used.
- Call for the product’s Marketing Authorization Holders (MAHs) to undertake risk assessments to identify the cause/s of nitrosamine contamination and put in place limits to ensure impurities fall below acceptable levels in a controlled manner.
- Request MAHs implement changes to guarantee that the future levels of nitrosamines are essentially absent.
Several different methods for determining nitrosamine impurities have been published by the FDA and the Official Medicines Control Laboratories (OMCLs) Network of the Council of Europe.
Highly Selective and Sensitive Method for Quantification of Nitrosamines in Valsartan Drug Substances

Valsartan and other related “sartan” drugs are frequently used to treat patients with hypertension or heart failure. However, since 2018, hundreds of recalls for sartans have been issued due to contamination with unacceptable levels of nitrosamines, a group of genotoxic compounds. Effective nitrosamine monitoring could help to ensure fewer of these costly product recalls, and unnecessary patient exposure. Download this app note to discover a method for quantifying nitrosamine levels in sartans.
Download App NoteSponsored Content
What drugs have been affected by nitrosamine impurities?
To date, nitrosamine impurities have been found in the various drugs listed below, which have subsequently been recalled by certain manufacturers.
Angiotensin II receptor blockers (ARBs) – Valsartan, Irbesartan and Losartan
Angiotensin II receptor blockers belong to the class of antihypertensive agents. They are used to treat hypertension and heart failure and selectively inhibit angiotensin II from binding to angiotensin II receptors on the muscles surrounding blood vessels, resulting in dilation and reduced pressure.
Valsartan
On July 13, 2018, the FDA issued a press release announcing the voluntary recall of several drugs containing valsartan, due to an impurity being detected. That impurity was NDMA. On July 27, 2018, the FDA released information on the levels of NDMA found in the recalled products. They also disclosed that, according to records supplied by the manufacturer, some levels of the nitrosamine impurity could have been present in the pharmaceutical products for as long as four years.
On September 13, 2018, the FDA announced that an additional impurity (NDEA) had been detected in three lots of recalled valsartan product. This fueled additional retesting of recalled products and additional testing of currently marketed drugs for the presence of NDEA.
Irbesartan
On October 30, 2018, the FDA released a statement warning of a voluntary recall of certain lots of irbesartan, because NDEA impurities had been detected. This was the first non-valsartan product detected by the agency as containing the NDEA impurity.
Losartan
On March 1, 2019, the FDA reported finding NMBA in specific lots of losartan and announces that 87 lots of medication were being recalled. Later the same day another release was issued announcing additional losartan product recalls due to the presence of NMBA impurities. Press releases were issued during April and June 2019, alerting patients and healthcare professionals to further recalls of losartan products.
The FDA has made available an updated list of all recalled angiotensin II receptor blockers.
Determination of Nitrosamine Impurities in Losartan Potassium Drug Substance Using Triple Quadrupole LC-MS
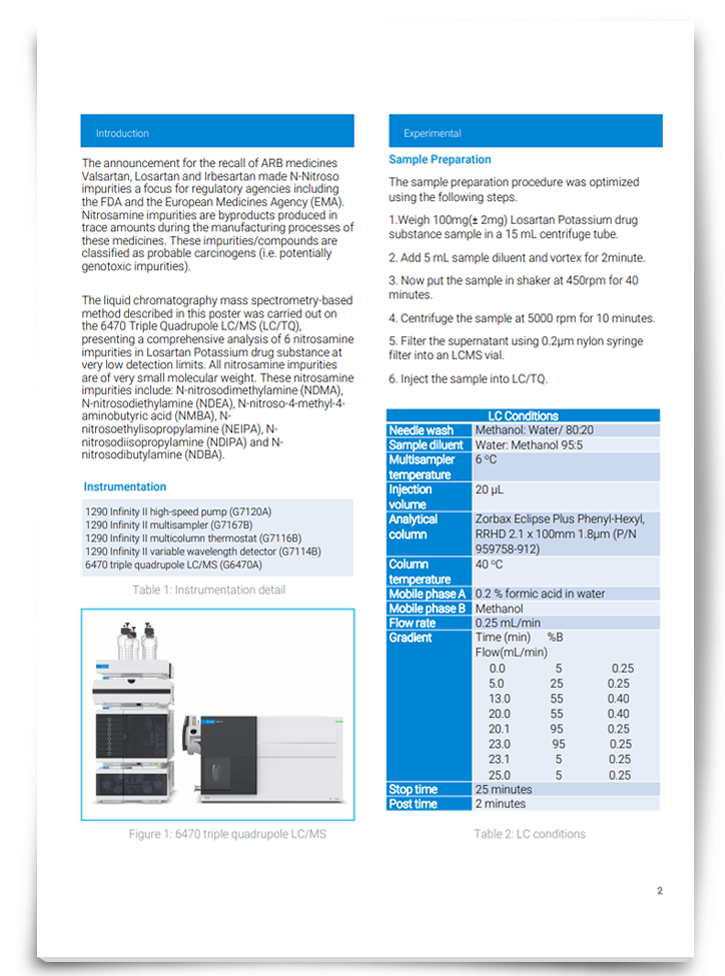
Nitrosamine impurities are byproducts produced in trace amounts during the manufacturing processes of angiotensin receptor blocking (ARB) medications. However, these impurities are classified as probable carcinogens, and so their discovery in and consequent recall of ARB drugs such as Losartan made N-Nitroso impurities a focus for many regulatory agencies. Download this poster to discover a method that can provide a comprehensive analysis of nitrosamine impurities.
Download PosterSponsored Content
Ranitidine and nizatidine
The drug ranitidine is a fast-acting histamine H2 receptor antagonist. It works by inhibiting secretion of gastric acid, lowering the volume of the acid and pepsin content of the secretion. Nizatidine is a potent histamine H2 receptor antagonist and works in a similar way to ranitidine.
On September 13, 2019, the FDA issued a press release announcing that NDMA impurities had been detected in some ranitidine medications. On the same date the EMA announced that it would begin reviewing ranitidine medicines following detection of NDMA. Over the following months, additional releases were issued announcing voluntary recalls of both ranitidine and nizatidine products.
The FDA has made laboratory analysis of ranitidine and nizatidine products available.
Metformin
Metformin is used to treat Type 2 diabetes mellitus, particularly in overweight individuals, when diet and exercise alone does not result in sufficient glycemic control. It works by lowering both basal and post-prandial plasma glucose.
On December 05, 2019, the FDA released a statement from Janet Woodcock, M.D., Director of FDA’s Center for Drug Evaluation and Research, in relation to the discovery of low levels of DNMA impurities in metformin drugs outside of the US. Exactly one month later the EMA acknowledged the presence of non-EU metformin medicines containing trace amounts of NDMA.
On May 28, 2020, the FDA announced that NDMA impurities above the acceptable intake limit had been detected in several lots of the extended-release (ER) formulation of metformin. In June 2020, the FDA alerted patients and healthcare providers that five companies were voluntarily recalling certain ER metformin products.
The FDA has made laboratory analysis of metformin products available.


