Blood Group of Donor Lungs Converted in Quest for Universal Organs
Complete the form below to unlock access to ALL audio articles.
Researchers from the Latner Thoracic Surgery Research Laboratories and University Health Network’s Ajmera Transplant Centre have converted the blood group of donor lungs in a step towards creating universal organs.
Blood group and transplant waiting times
Every individual belongs to a particular blood group that is determined by the genes we inherit from our parents. We can identify which blood group we belong to by analyzing the antigens and antibodies present in our blood.
Understanding blood groups
- Blood group A – possess A antigens on red blood cells, with anti-B antibodies in their plasma
- Blood group B – possess B antigens on red blood cells, with anti-A antibodies in their plasma
- Blood group O – possess no antigens, with anti-A and anti-B antibodies in their plasma
- Blood group AB – possess both A and B antigens, and have neither anti-A nor anti-B antibodies in their plasma
Blood group: | Can donate blood to the following blood groups: |
| A | A, AB |
| B | B, AB |
| Type AB | AB |
| Type O | O, A, B, AB |
Understanding which blood group we belong to is important, should we ever require a blood transfusion. Donor blood must possess the same antigens as the recipients – or no antigens, as in blood group O – to prevent an immune response being triggered by foreign antigens.
Antigens A and B are also found on the surface of blood vessels in our organs, which means that our blood group also determines who we can donate to and receive organ transplants from. Among other tests, blood group determination is a key step for “matching” a donor organ to a potential recipient. If an individual possesses anti-A and anti-B antibodies in their blood stream, like blood group O, they can only receive an organ from a donor that is also blood group O; otherwise, the organ would likely be rejected.
“For every candidate on the transplant waiting lists, blood type compatibility is one of the key criteria to consider when matching a donor organ. The respective donor pool for each patient differs depending on their blood type, leading to longer waiting times and higher death rates while waiting for certain patients,” Dr. Marcelo Cypel, thoracic surgeon at the University Health Network (UHN) and professor of surgery at the University of Toronto, told Technology Networks.
Over recent years, a growing body of research has explored the possibility of generating “universal type O organs”, which would overcome the issue of allocating organs based on blood group, reducing waiting times for patients on the transplant list. In a new collaborative study published in Science Translational Medicine, Cypel and colleagues across several organizations in Canada have taken one step closer to this notion becoming a reality. In a proof-of-concept experiment, they demonstrated that it was possible to convert donor lungs to a universal blood group.
Towards “universal” organs
The research relied on previous work conducted by Professor Stephen Withers, a biochemist from the University of British Columbia, who identified a group of enzymes capable of clearing antigens.
“The enzymes that remove the A antigen were discovered using the technique of metagenomic screening,” said Withers. “This approach allows us to take all the genes (DNA) from all the bacteria in a particular sample – in this case the feces of a donor of AB blood type – and place each of those bits of DNA into a different Escherichia coli (E coli) bacterium, creating a ”collection” or “library” of E coli where each of them can hopefully “read” the DNA placed in it and produce the corresponding protein.”
Most of the DNA will not be successfully “read” or make the enzyme of interest, so Withers and colleagues screen the large libraries using high-throughput methods, to identify the enzyme of interest. “In this case, we found a pair of enzymes that were by far the most active of all those we tested and together they cleaved off the single sugar (N-acetylgalactosamine, or GalNAc for short) that defines the A antigen,” he explained. When GalNAc is cleaved off, the A antigen is converted to the H-antigen, the antigen found in group O blood or tissues.
“We then tested these enzymes on red blood cells (RBCs) and found they worked extremely well and efficiently convert them to type O RBCs. We are pursuing the potential of this approach for broadening the blood supply,” explained Withers. In parallel, he began to work in collaboration with Dr. Cypel and Dr. Aizhou Wang, a postdoctoral research fellow in Cypel’s lab, to understand the potential application in solid organs.
Using the EVLP system and enzymes to treat donor lungs
In the Cypel lab, the researchers obtained human donor lungs that had been deemed unfit for transplant from group A donors. “The ex vivo lungs used in this experiment are donor lungs that were deemed non-suitable for transplant and consented for research. The age and sex of the donors span from ages 28 to 78 and an approximately equal distribution of male and female,” Wang told Technology Networks.
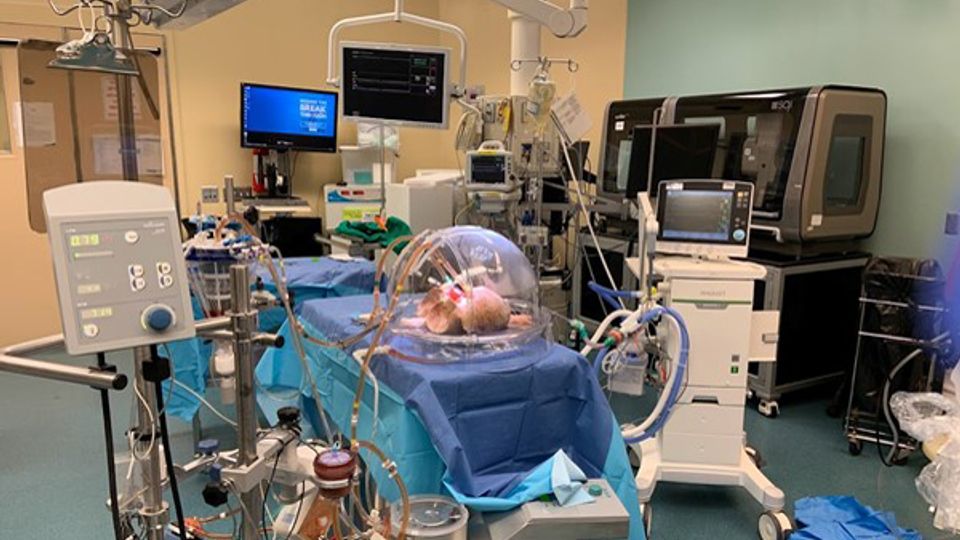
The researchers used a system pioneered in Toronto, known as ex vivo lung perfusion, or EVLP. The EVLP platform that can pump fluids through organs, keeping them at body temperature such that they can be modified prior to transplantation.
The A group donor lungs were placed in the EVLP circuit. One lung of each pair utilized was treated with enzymes to cleave the antigens, while the other lung – obtained from the same donor – was left untreated as a control.
The researchers then added type O blood to the circuit, which, under normal circumstances, would instigate signs of rejection of the organ. The team found that the lungs treated with the enzyme tolerated the O group blood well, while the donor lungs that were untreated started to show biological signs of rejection.
“In an ABO-incompatible transplant, rejection is kicked off by anti-donor specific antibodies recognizing the foreign antigens. This process activates the complement system, which is part of the immune system, and elicits inflammation, ultimately causing lung function to fail,” described Wang. “In our study, we tried to follow this process closely by monitoring antibody binding, signs of complement activation via complement deposition, inflammation and lung function, so we can understand better the impact of the treatment on the process of rejection.”
It's important to note that the ex vivo nature of the study prevents the research team from gaining a full picture of how the converted lungs would be affected by the immune system in vivo, such as in a transplant recipient.
Next steps: Moving towards a clinical trial
Based on the success of their proof-of-concept study, the research team are now in planning mode for a safety clinical trial, though they are unable to share any more information at this stage. Cypel emphasizes that, while this study was conducted on lungs as an example, studies on other solid organs are also underway.
Transplantations can be a costly endeavor for healthcare systems and patients. Technology Networks asked how the method of conversion could impact the costs of transplant procedures. “While this treatment may add cost to transplantation, it can also offset costs related to patients in hospital or critical care that are waiting for a suitable donor organ,” Wang concluded.
Dr. Marcelo Cypel, Professor Stephen Withers and Dr. Aizhou Wang were speaking to Molly Campbell, Senior Science Writer for Technology Networks.
Reference: Wang A, Ribeiro R, Ali A et al. Conversion of blood type A donor lungs into universal blood type lungs using ex vivo ABO enzymatic treatment. Sci Trans Med. 2022. doi: 10.1126/scitranslmed.abm7190.


