Laser-based Imaging System Teams Up With Algorithm To Identify Brain Tumors
Complete the form below to unlock access to ALL audio articles.
A novel method of combining advanced optical imaging with an artificial intelligence algorithm produces accurate, real-time intraoperative diagnosis of brain tumors, a new study finds.
The study examined the diagnostic accuracy of brain tumor image classification through machine learning, compared with the accuracy of pathologist interpretation of conventional histologic images. The results for both methods were comparable: the artificial intelligence–based diagnosis was 94.6 percent accurate, compared with 93.9 percent for the pathologist-based interpretation.
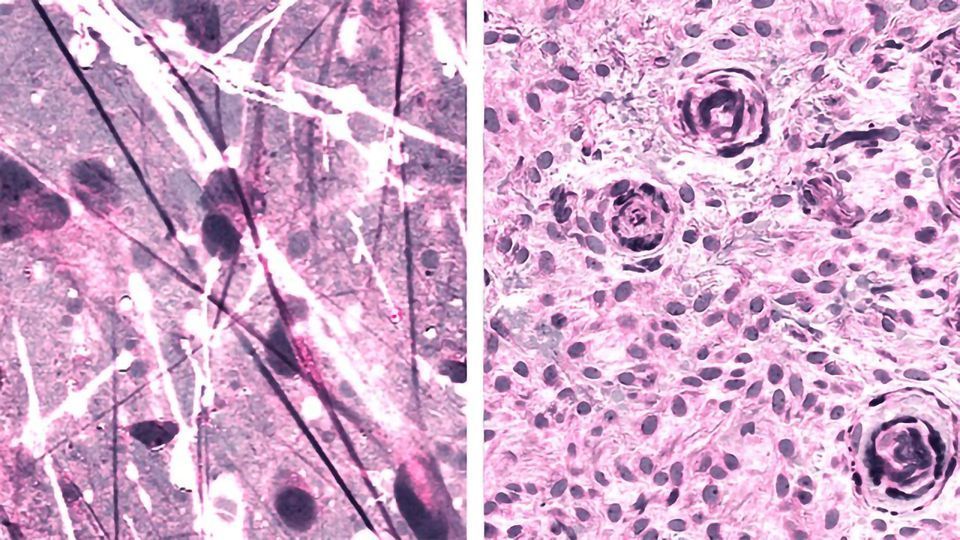
The imaging technique, stimulated Raman histology (SRH), reveals tumor infiltration in human tissue by collecting scattered laser light, illuminating essential features not typically seen in standard histologic images.
The microscopic images are then processed and analyzed with artificial intelligence, and in under two and a half minutes, surgeons are able to see a predicted brain tumor diagnosis. Using the same technology, after the resection, they are able to accurately detect and remove an otherwise undetectable tumor.
“As surgeons, we’re limited to acting on what we can see; this technology allows us to see what would otherwise be invisible, to improve speed and accuracy in the OR, and reduce the risk of misdiagnosis,” says senior author Daniel A. Orringer, MD, associate professor in the Department of Neurosurgery at NYU Langone, who helped develop SRH and co-led the study with colleagues at the University of Michigan. “With this imaging technology, cancer operations are safer and more effective than ever before.”
How the study was conducted
To build the artificial intelligence tool used in the study, researchers trained a deep convolutional neural network (CNN) with more than 2.5 million samples from 415 patients to classify tissue into 13 histologic categories that represent the most common brain tumors, including malignant glioma, lymphoma, metastatic tumors, and meningioma.
In order to validate the CNN, researchers enrolled 278 patients receiving brain tumor resection or epilepsy surgery at 3 university medical centers in the prospective clinical trial. Brain tumor specimens were biopsied from patients, split intraoperatively into sister specimens, and randomly assigned to the control or experimental arm.
Specimens routed through the control arm—the current standard practice—were transported to a pathology laboratory and went through specimen processing, slide preparation by technicians, and interpretation by pathologists, a process which takes 20 to 30 minutes. The experimental arm was performed intraoperatively, from image acquisition and processing to diagnostic prediction via CNN.
Notably, the diagnostic errors in the experimental group were unique from the errors in the control group, suggesting that a pathologist using the novel technique could achieve close to 100 percent accuracy. The system’s precise diagnostic capacity could also be beneficial to centers that lack access to expert neuropathologists.
“SRH will revolutionize the field of neuropathology by improving decision-making during surgery and providing expert-level assessment in the hospitals where trained neuropathologists are not available,” says Matija Snuderl, MD, associate professor in the Department of Pathology at NYU Langone and a co-author of the study.
Reference
Hollon et al. (2020) Near real-time intraoperative brain tumor diagnosis using stimulated Raman histology and deep neural networks. Nature Medicine. DOI: https://doi.org/10.1038/s41591-019-0715-9
This article has been republished from the following materials. Note: material may have been edited for length and content. For further information, please contact the cited source.

